Yes, compression socks can help manage Restless Legs Syndrome (RLS) by improving blood circulation and reducing leg discomfort. Medical-grade compression socks with 15–20 mmHg pressure often ease tingling, burning, and the urge to move, especially at night, improving sleep quality.
What is Restless Leg Syndrome (RLS)?
Medically known as Willis-Ekbom Disease, Restless Leg Syndrome (RLS) is a neurological sensorimotor disorder that creates an overwhelming urge to move your legs, often accompanied by uncomfortable sensations. This condition affects between 5% and 10% of Americans, with approximately 1.5 million children and adolescents experiencing symptoms as well. For many sufferers, finding relief becomes a constant challenge, leaving many wondering if treatments like compression socks for restless leg syndrome might provide comfort.
Common symptoms and sensations
RLS manifests through a variety of uncomfortable sensations that make sitting or lying still nearly unbearable. These sensations include:
- Tingling or burning feelings
- Creeping or crawling sensations
- Throbbing or aching
- Itching or pulling sensations
- Pain (reported by 59.4% of RLS sufferers)
What makes RLS unique is the intense, irresistible urge to move that accompanies these sensations. As one neurologist describes it, patients experience “an irresistible urge to move their legs and an inability to sit or lie still”. Moreover, movement temporarily relieves the discomfort, only for symptoms to return once movement stops.
When and why symptoms appear
RLS symptoms follow a distinct pattern that differentiates it from other conditions. Notably, symptoms:
- Worsen during periods of rest or inactivity
- Intensify in the evening or at night
- Improve with movement
- Often affect both sides of the body equally
The exact cause of RLS remains somewhat mysterious, though research points to dysfunction in the brain’s basal ganglia, which uses dopamine to regulate movement. Furthermore, certain factors can contribute to RLS development, including genetics (RLS often runs in families), iron deficiency, certain medications, and underlying medical conditions.
How RLS affects daily life and sleep
Perhaps the most destructive aspect of RLS is its profound impact on sleep and daily functioning. Sleep disturbance represents a cardinal feature of RLS, with over two-thirds of patients experiencing serious insomnia. Consequently, many report taking more than 30 minutes to fall asleep and waking up at least three times nightly.
This chronic sleep disruption creates a cascade of daytime effects:
- Daytime fatigue and exhaustion (reported by 47.6% of sufferers)
- Difficulty concentrating and memory problems
- Mood changes and irritability (affecting 50.5% of patients)
- Decreased productivity and disrupted daily activities (reported by 40.1% of sufferers)
- Depression and anxiety
“Whether awake or asleep, the RLS patient finds little opportunity for the general restorative behaviors necessary for healthy human functioning,” notes one study. This ongoing sleep deprivation can worsen RLS symptoms, creating a vicious cycle as lack of sleep further disrupts dopamine regulation.
For those with moderate to severe RLS, symptoms can occur twice weekly or more, significantly diminishing quality of life. Understanding these impacts helps explain why many patients eagerly explore various treatment options, including whether compression socks help RLS symptoms by improving circulation and potentially addressing the underlying discomfort.
What Causes RLS and Who is at Risk?
The underlying causes of RLS remain partially mysterious, yet research has uncovered several key factors that contribute to this challenging condition. Understanding these causes helps explain why some people might find relief from compression socks for restless leg syndrome while others need different approaches.
Dopamine imbalance and brain function
At its core, RLS appears linked to disruptions in brain chemistry. Scientists believe that dysfunction in the brain’s dopamine signaling plays a central role. This neurotransmitter helps control smooth, purposeful muscle movement through the basal ganglia—a part of the brain that regulates movement. When dopamine pathways don’t function properly, involuntary movements often result.
Interestingly, this dopamine connection explains why RLS symptoms tend to worsen at night. The brain’s dopamine levels naturally fluctuate throughout the day, reaching their lowest point in the evening—precisely when RLS symptoms typically intensify. This also explains why medications that stimulate dopamine often help reduce symptoms, while those that block dopamine can worsen them.
Some research suggests peripheral blood flow problems might also contribute to RLS symptoms. One hypothesis proposes that peripheral hypoxia (insufficient oxygen) creates the urge to move to improve tissue oxygenation. This circulation theory helps explain why some patients report improvement with compression socks for RLS.
Nutrient deficiencies and medical conditions
Several key nutrient deficiencies have been strongly linked to RLS development:
- Iron deficiency: Perhaps the most significant nutritional link to RLS, iron deficiency affects dopamine production in the brain. Studies show decreased brain/CSF measures of iron in people with RLS, and iron treatments often improve symptoms. People with iron deficiency anemia have a very high RLS prevalence of 25-35%.
- Vitamin D deficiency: Research indicates significantly lower vitamin D levels in people with RLS compared to those without the condition. Furthermore, more severe vitamin D deficiency correlates with more severe RLS symptoms and worse sleep quality.
- B12 and magnesium deficiencies: Low levels of vitamin B12 and magnesium have been linked to a higher risk of RLS flare-ups. B12 deficiency may lead to decreased production of enzymes involved in dopamine metabolism.
Medical conditions often associated with RLS include kidney disease, diabetes, peripheral neuropathy, and Parkinson’s disease. In fact, as many as half of people with Parkinson’s disease also have RLS, highlighting the dopamine connection between these conditions.
Pregnancy, genetics, and lifestyle triggers
RLS frequently runs in families, suggesting a strong genetic component. Specific gene variants have been identified as risk factors, with the MEIS1 gene showing the largest effects.
Pregnancy dramatically increases RLS risk, with about one-fourth of pregnant women developing symptoms, usually in the third trimester. Hormonal changes, increased blood volume, and the pressure of the growing uterus likely contribute. Notably, about 60% of women who experience RLS during one pregnancy will have it again during subsequent pregnancies.
Numerous lifestyle factors can trigger or worsen symptoms:
- Alcohol and caffeine consumption
- Certain medications, especially antihistamines, antidepressants, and anti-nausea drugs
- Prolonged inactivity, such as long flights or sitting still for extended periods
- Stress and sleep deprivation
Understanding these causes and risk factors helps explain why treatments like compression socks for RLS might work for some people—especially those with circulation issues—but why a comprehensive approach addressing multiple factors often yields the best results.
How Compression Socks Help with RLS
Many RLS sufferers have found surprising relief through a simple, non-invasive approach. Compression socks—specialized garments that apply graduated pressure to the legs—offer a science-backed method for alleviating those frustrating RLS symptoms that keep you up at night.
Improving blood flow and circulation
Compression therapy works by applying controlled pressure to your lower extremities, which helps increase blood circulation throughout your legs, ankles, and feet. This improved circulation is particularly beneficial for RLS sufferers since inadequate blood flow can worsen those uncomfortable sensations.
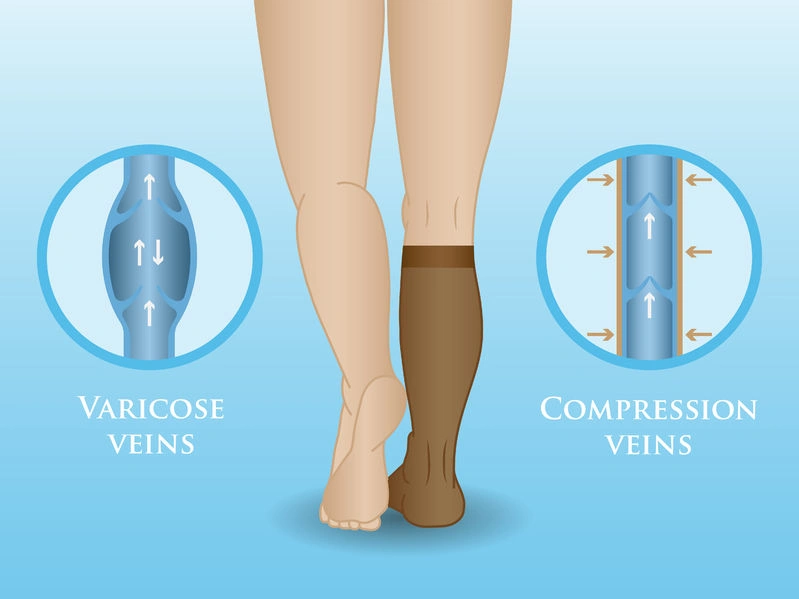
The science behind compression is straightforward yet effective. These socks apply graduated pressure—tightest around the ankles and gradually decreasing up the leg. This pressure gradient helps push blood from the superficial veins into the deep veins, keeping blood flowing efficiently toward your heart. As a result, your arteries can relax, allowing oxygen-rich blood to flow more freely to leg muscles.
Studies suggest that enhanced circulation plays a significant role in reducing leg discomfort associated with RLS. By improving blood flow, compression socks help deliver more oxygen to your leg tissues, which may help calm the nerve sensations that trigger RLS symptoms.
Reducing nerve irritation and discomfort
Beyond improved circulation, compression socks address another critical aspect of RLS—nerve irritation. The steady, even pressure they provide can help quiet the sensations that make RLS so disruptive.
Many users describe the feeling as a gentle “hug” for their legs, which provides a soothing effect on irritated nerves. This consistent pressure helps counteract the tingling, crawling, or pulling sensations characteristic of RLS.
Research from 2017 indicates that some individuals experience symptom relief through mechanical stimulation provided by pressure. Although not specific to compression socks, they offer a similar pressure-based mechanism that benefits those with RLS.
Preventing blood pooling in the legs
One of the most significant benefits of compression therapy for RLS sufferers is preventing blood from pooling in the lower legs—a condition often associated with venous insufficiency.
Compression socks work by mimicking the natural movements your body makes when pumping blood from your legs back to your heart. By squeezing your lower legs, the socks prevent blood from collecting in the veins and help reduce fluid buildup.
This mechanism is particularly helpful since:
- It decreases leg swelling that can exacerbate RLS discomfort
- It aids proper circulation by offsetting blood pooling from weakened vein valves
- It helps push fluid out of your legs, reducing inflammation
A study involving pregnant women with RLS found that compression stockings reduced symptom severity, with effects starting in approximately 3.93 days on average. The effectiveness of compression stockings in relieving RLS symptoms supports the theory that the condition may be associated with venous insufficiency.
Although compression socks aren’t a cure for RLS, they represent a valuable tool in managing symptoms. For many sufferers, they provide noticeable relief, particularly when combined with other treatments. Their ability to address multiple potential contributors to RLS—from poor circulation to nerve irritation—makes them worth considering as part of your approach to managing this challenging condition.
Choosing the Right Compression Socks for RLS
Finding the perfect pair of compression socks for RLS means understanding three critical factors that determine their effectiveness. Indeed, not all compression socks deliver the same benefits, and making the right choice can significantly impact your symptom relief.
Compression levels: mild vs. medical-grade
The pressure level is perhaps the most essential consideration for compression socks that actually help with RLS symptoms:
- Mild to moderate compression (15-20 mmHg) works well for most people with RLS, providing enough pressure to improve circulation without discomfort. This level effectively supports blood flow while remaining comfortable enough for extended wear.
- Medical-grade compression (20-30 mmHg) offers stronger pressure typically reserved for treating serious conditions like severe varicose veins. For RLS, this higher level should generally only be used under medical guidance.
Graduated compression—tighter at the ankle and gradually decreasing upward—helps push blood toward your heart more effectively than uniform pressure. This design fundamentally mimics natural muscle contractions that facilitate healthy circulation.
Length and material considerations
Choosing the right style and fabric can make a substantial difference in comfort:
- Knee-high socks are generally the most practical choice for RLS sufferers. They target the lower leg area most affected by RLS symptoms without feeling overly restrictive during sleep.
- Thigh-high or pantyhose styles provide additional coverage yet may feel too constrictive for nighttime use.
Regarding materials, look for:
- Breathable, moisture-wicking fabrics if you’ll wear them overnight
- Cotton blends or specially designed “sleep compression” socks for softer feel
- Smooth, non-binding top bands to prevent the socks from digging into your skin
How to measure for a proper fit
Properly, the effectiveness of compression socks depends heavily on fit—too loose won’t provide enough support, while too tight can be counterproductive or even harmful.
For accurate measurements:
- Measure first thing in the morning when swelling is minimal
- Take measurements against bare skin, not over clothing
- Measure your ankle circumference at the narrowest point
- Measure your calf at its widest point
- For knee-high socks, measure from the floor to the bend of your knee
Compare these measurements carefully with sizing charts before purchasing. Remember that compression sock sizing often differs from regular sock sizing.
If you’re between sizes, it’s typically better to size up rather than down. The socks should feel snug but never painful—they should never cause numbness, tingling, or excessive redness.
Best Practices for Using Compression Socks
Knowing how to properly use compression socks can dramatically improve their effectiveness for RLS symptom management. Following these evidence-based practices helps maximize relief and comfort.
When to wear them for maximum benefit
Timing matters tremendously with compression therapy for RLS. Most sufferers experience maximum benefit by wearing their compression socks in the evening hours when symptoms typically intensify. Putting them on a few hours before bedtime helps prevent the uncomfortable sensations that disrupt sleep. Some users report wearing them during particularly inactive periods—while watching TV, during long flights, or when working from desk.
For newcomers to compression therapy, gradual adaptation works best. Start by wearing them for just 1-2 hours initially, gradually increasing duration as your body adjusts. Consistency proves key—regular, steady use gives your body the best chance to adapt and experience long-term improvements.
Combining with stretching and movement
Pairing compression therapy with gentle movement creates a powerful combination. Simple calf stretches, yoga poses, or brief walks before bedtime complement the circulatory benefits of compression socks. This combination relaxes tense muscles while simultaneously improving blood flow.
Many RLS sufferers additionally benefit from warm soaking baths before bed to relax muscles. For those with severe symptoms, alternating warm and cool packs occasionally provides extra relief by promoting blood flow and reducing limb sensations.
Signs you may need professional guidance
Despite their effectiveness, compression socks aren’t appropriate for everyone. Seek medical advice immediately if you have diabetes, severe arterial disease, or skin ulcers. Furthermore, persistent or worsening symptoms despite compression therapy might indicate underlying venous insufficiency requiring proper vascular evaluation.
Your healthcare provider can recommend appropriate compression strength and fit specifically for your condition. This personalized guidance ensures you’re using the right approach for your unique situation.
Conclusion
Restless Leg Syndrome significantly impacts daily life and sleep quality for millions of Americans. Though compression socks certainly cannot cure RLS completely, they offer a practical, non-invasive option for symptom management. The graduated pressure these specialized garments provide works primarily through improved circulation, reduced nerve irritation, and prevention of blood pooling—all factors that can trigger or worsen RLS symptoms.
Finding relief starts with selecting the right compression level. Most RLS sufferers benefit from mild to moderate compression (15-20 mmHg), while proper fit remains essential for effectiveness. Knee-high socks generally work best, balancing coverage with comfort for nighttime wear.